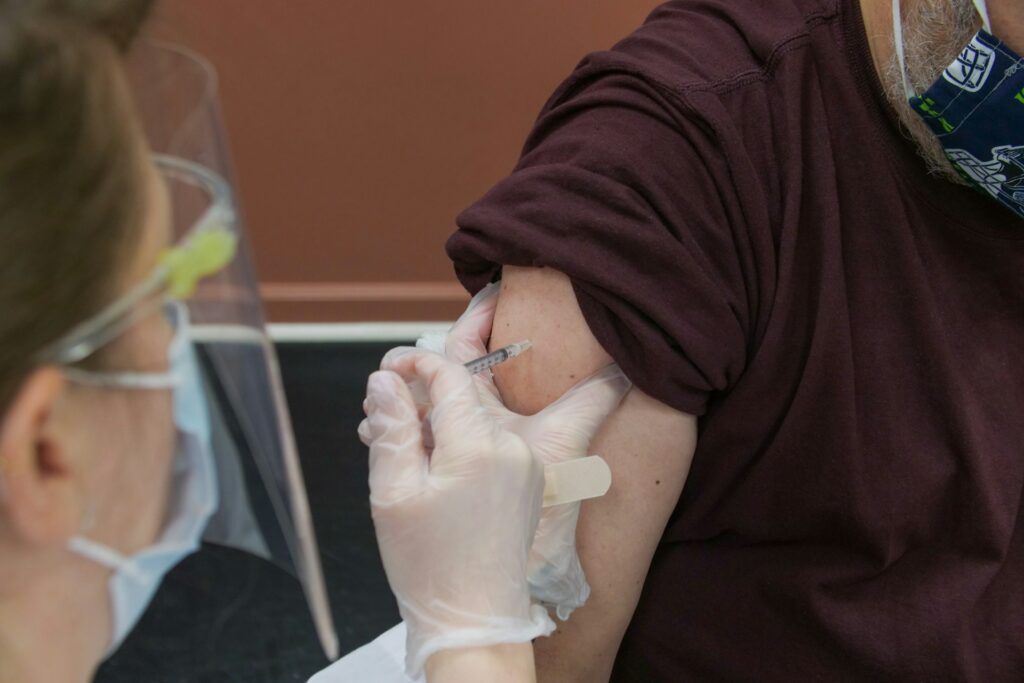
What is the value of a treatment?
As of July, the U.S. government has given out close to 600 million doses of COVID-19 vaccines at prices that ranged between $15-$20 per dose, which means they spent $10-$12 billion on shots. Research shows that, as of March, the U.S. vaccination program saved 2 million lives and $900 billion in health care costs, while preventing 17 million hospitalizations. There were also massive economic benefits from ending lockdowns and getting people back to work.
Suffice it to say the U.S. government got good value.
The Senate’s current plan to establish government controls on drug prices is illogical simply because the price of prescription drugs is growing slower than inflation. But when you look at the situation through the lens of value for care, the true harm that the plan could do to the U.S. economy and society becomes clear. While public and private insurers make payments for medical care, there is wide recognition among government, researchers, and industry that we need to follow a value-based health care approach, which makes patients the ultimate determiners of the value of health care.
“Consider the impact of government-mandated price controls from a patient’s point of view: What does the prospect of reduced revenue do for the future of investment and future development?” asks Daniel Durham, Senior Health Policy Advisor, of the Biotechnology Innovation Organization (BIO). “How many therapies won’t be developed now that could cure patients?”
Value-based health care
As Durham explains, the price of a treatment is only one component of the more important concept of the value of a treatment. Advocates of health care reform, especially patient groups, say we need to adjust our focus to achieve care that has the highest value for patients and their families.
A value-based care approach puts patients at the center of health care by ensuring that “hospitals and physicians are paid based on patient health outcomes,” according to a New England Journal of Medicine brief. “Under value-based care agreements, providers are rewarded for helping patients improve their health, reduce the effects and incidence of chronic disease, and live healthier lives in an evidence-based way.”
It is a simple concept that is hard to execute, but it offers a better means for distributing our limited health care resources.
While we have a complex health care system with a broad array of actors and stakeholders, the ultimate goal is “to support a single endeavor: to provide care that maximizes the health and well-being of each patient as effectively and efficiently as possible. This objective is the common thread running through every part of the health care system, connecting all of the stakeholders it affects,“ according to Jennifer Bright and Alan Balch.
Bright and Bach write the summation of a 12-part series on the challenges of assessing the value of health care, produced by the Innovation and Value Initiative (IVI). IVI’s mission is to champion a focus on patient-centered outcomes in health interventions. Guided by a Scientific Advisory Panel and a Patient Advisory Council, IVI pursues its mission through research, advocacy, and efforts to engage patients and promote health equity.
Avoiding discriminatory value judgements
Fostering a system based on the true value of care is a challenge, and some efforts to quantify value are criticized for being insufficiently sophisticated—or based on the wrong values. One organization in this field is the Institute for Clinical and Economic Review (ICER).
According to Durham, ICER tries to focus on the results for “the average patient. But there is, in reality, no average patient.” Durham gives an example of how averages might create a tendency to ignore drugs with real potential to help many people: “In a trial for a cancer drug, the average may show that progression-free survival is six months, however for 20% of the patients, it’s 10 years.”
One of the metrics ICER uses is the Quality Adjusted Life Year (QALY), which is an attempt to combine the number of years a treatment adds to a person’s life with the quality of their health during those years. Unfortunately, because they give greater value to a “healthy” life, QALYs make judgments about whose life is more important.
“QALY is very discriminatory. If you’re disabled, you’re downgraded,” said Durham. “The National Council on Disability has said that QALY is discriminatory.”
The QALY system is inappropriate for judging cancer treatments, Dr. William Smith writes for the Pioneer Institute. He notes that a QALY would give a poor rating to a treatment that extends a patient’s life by only a few months, but the patient might give very high value to a few more months of life. As another example, treatments that reduce the amount of care a patient needs provide an indirect social benefit by freeing up that person’s carer.
“The reason that ICER does not include the clear societal benefits of certain treatments is obvious: consideration of such data would result in more treatments being rated as cost effective,” Dr. Smith argues.
Lessons from the pandemic
We have learned a lot about how to value care from dealing with COVID-19, according to IVI contributors Darius N. Lakdawalla, Mark T. Linthicum, and Charles Phelps. For one thing, we learned that we must treat value as a societal issue, understanding that, for example, getting everyone out of pandemic lockdown and back to work was a huge value for society that should be included in our measurements of value.
Another lesson of COVID-19 is the need to focus on patients, a widely diverse group with different needs and concerns. This involves using novel approaches to learn about patient’s treatment goals and expectations—as well as their fears of treatment. It also involves being sure that clinical trials involve members of all groups in society so that they are truly representative and give data that is relevant to everyone.
A third lesson that Lakdawalla, Linthicum, and Phelps take from COVID-19 is the value patients and society place on reducing risk. While COVID-19 vaccines did not definitively prevent any infections, they reduced risks of serious disease, allowing us to change our assumptions when making decisions about returning to work.
Achieving value-based care
“Value in health care remains an elusive goal,’” write IVI’s Bright and Balch. Still, they argue that we are making some progress and can do more: “Through policies for funding and grantmaking, organizations such as the National Institutes of Health, Patient-Centered Outcomes Research Institute, and private foundations can further encourage research focused on patient-centered value or collection of relevant evidence.”
As with any market, the most powerful leverage is with the customer, who must demand what they want, according to Bright and Balch. Patients, and their employers who pay for insurance, need to make it clear to care providers and payers what value means to them, and they need to insist on receiving that value.
When government drug price controls discourage investment in future drug development, “there’s a tremendous loss of value there for patients who don’t yet have a therapy to treat their particular disease,” according to Durham.
That is why, he argues, patients, not the government, should determine the value of treatments.