Another tick-driven disease has found its way into existence: alpha-gal syndrome, which is thought to begin with the bite of a Lone Star tick and causes a unique allergic reaction to red meat.
While uncommon, this meat allergy has been gaining attention in recent years, especially as the range of the tick responsible is spreading due to changing climates.

What is alpha-gal syndrome?
Alpha-gal (from galactose-alpha-1,3-galactose) is found in tissues of non-primate mammals such as cows, pigs, sheep, and bison.
According to the Centers for Disease Control and Prevention (CDC), Lone Star ticks (Amblyomma americanum) introduce a sugar, or alpha-gal molecule, into the individual’s bloodstream via a bite. This bite triggers an immune response that can eventually lead to a syndrome.
If exposed to this molecule from a tick bite, the individual’s immune system becomes sensitized, leading to the production of antibodies against it.
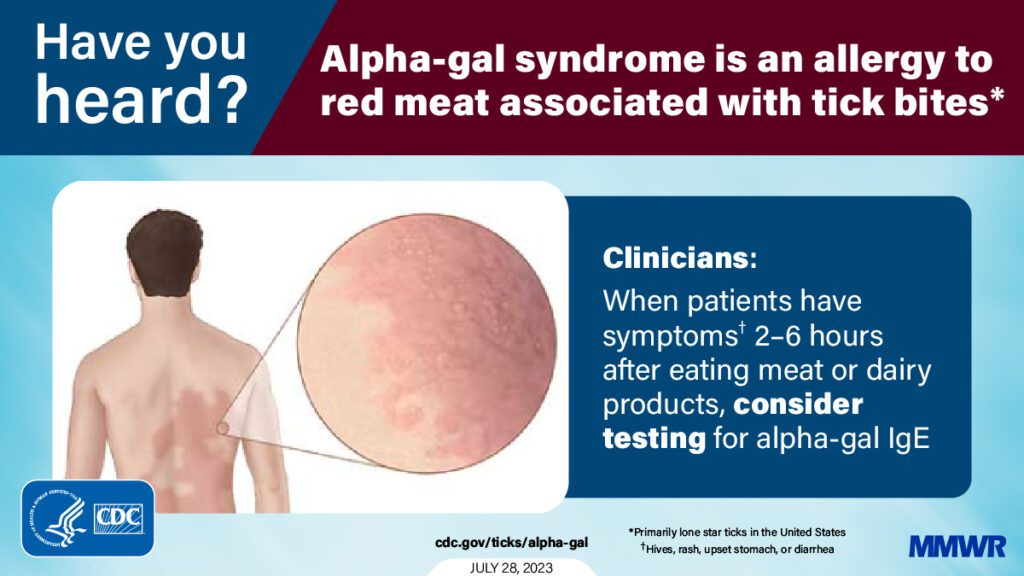
A distinct feature of this specific allergic reaction is that it does not occur immediately after the bite. It has a delayed onset, typically 3-6 hours after exposure. Symptoms occur hours after ingesting the red meat. Cases have been reported with beef, pork, lamb, organ meats, gelatins, or dairy products from mammals.
Symptoms include hives, pruritis (or itching), edema (or swelling), shortness of breath, abdominal pain, nausea, vomiting, or diarrhea. Severe cases causing anaphylaxis have been documented and can be fatal.
What makes alpha-gal syndrome different than other tick-driven diseases?
Unlike Lyme disease, which is most frequently reported in the northeastern, mid-Western, and mid-Atlantic U.S., alpha-gal has been identified most often in the southeastern U.S., where Lone Star ticks are found.
The CDC reported >110,000 cases of alpha-gal syndrome between 2010 and 2022, though they suspect cases are significantly under-reported, estimating nearly 450,000 individuals have been infected since 2010.
The only treatment is to manage symptoms conservatively with antihistamines or corticosteroids. Anaphylaxis would require hospitalization and IV epinephrine.
Protecting oneself from exposure to ticks is also important as new tick bites may reactivate allergic reactions into alpha-gal syndrome.
As potentially life-threatening, avoidance seems to be key. But given its potential array of exposure, avoiding alpha molecules is not as easy as becoming a vegetarian.
The success in managing alpha-gal syndrome is in having a high index of suspicion and taking action. The delayed reaction is likely related to the time it takes the alpha molecules to not only be digested but to enter the bloodstream. A detailed medical history, a thorough physical exam, and an alpha-gal IgE blood test will indicate a diagnosis.
Until a cure is found, research is underway to pinpoint the mechanism behind the delayed onset of symptoms, the role of tick saliva in sensitization, and possible methods for prevention and treatment.



