Along with climate change comes longer, warmer months, which means an extended tick season. With more time spent outdoors, there’s an inevitable increase in tick-borne illness. Given its debilitating symptoms and potential long-term complications, Lyme disease awareness has never been more important as it is a growing public health concern.
Most commonly caused by the bacterium Borrelia burgdorferi, Lyme disease is transmitted to humans primarily via bite of an infected deer tick. This black-legged tick has become rampant in wooded and grassy areas within endemic areas of the United States, including the Northeast, mid-Atlantic, upper Midwest, and the West Coast.
How do you know if you’ve been bit?
Diagnosis is not straightforward as symptoms are nonspecific. Early signs and symptoms of Lyme disease, occurring within days and weeks of a tick bite, include fever, chills, headache, fatigue, joint and muscle aches, and swollen lymph nodes.
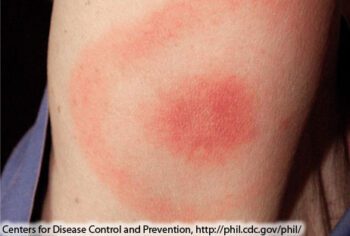
The appearance of a rash, or Erythema migrans (EM), appears in approximately 75-80% of infected patients. The rash may feel warm but is rarely itchy or painful. Coloration varies but often appears to resemble a “bull’s eye.” The rash would be found at the site of the tick bite within 7-30 days and would gradually expand up to a size of 30 cm in some cases. Given bites may occur anywhere on the body, including the scalp, identification or inclusion of a rash is not mandatory to make a diagnosis.
Late signs and symptoms, occurring months after a tick bite, may include severe headaches, nerve pain, neck stiffness, facial paralysis, pain and swelling of the joints, tendons, muscles, and bones, numbness and tingling of the extremities, palpitations, dizziness, shortness of breath, and additional rashes aside from EM.
Medical assessment of a potential tick infection includes medical history, clinical presentation, and laboratory tests. Definitive testing is a two-step process which includes serology to detect antibodies against the bacteria in the form of an enzyme immunoassay (EIA) and western blot. False negatives test results may occur during early stages of the illness.
Have a high index of suspicion
 If you have symptoms and you can pinpoint specific times you have spent outdoors in high grass or woody areas, having a high index of suspicion can help with timely treatment and prevent progression of Lyme disease. Identification and removal of the entire tick is essential to ensure proper eradication of the bacteria.
If you have symptoms and you can pinpoint specific times you have spent outdoors in high grass or woody areas, having a high index of suspicion can help with timely treatment and prevent progression of Lyme disease. Identification and removal of the entire tick is essential to ensure proper eradication of the bacteria.
This requires close inspection, grasping the tick by its head close to the skin with a tweezer, and gently pulling traction for its removal. Concern of not being able to remove an embedded or entire tick is justification to seek medical attention. Early detection and timely treatment are imperative for effective management.
The primary treatment, if given within a timely fashion, is effective and includes a 2-4 week course of antibiotics, such as doxycycline, amoxicillin, or cefuroxime. Advanced disease or persistent symptoms may require longer treatment and/or hospitalization for IV therapy, such as ceftriaxone.
Long-standing symptoms of Lyme disease
Cases of chronic Lyme disease have increased over the past decade, and discussions regarding proper treatment amongst the medical community have raised criticism and debate. In 2002, the LYMErix vaccine was marketed in the United States but discontinued by the manufacturer following insufficient consumer demand. In 2015, the Centers for Disease Control and Prevention (CDC) announced the development of a new vaccine by Valneva and Pfizer, called VLA15, which is currently in Phase 3 clinical trials.
There are also reports of a human monoclonal antibody being developed as a pre-exposure prophylaxis which would provide seasonal protection for Lyme disease. Research is still underway.
Prevention is key
Preventing Lyme disease begins with an awareness of its presence. The black-legged ticks are small and often difficult to detect. Protective clothing that includes long sleeves, pants, and closed-toed shoes, and insect repellents containing DEET or picaridin should be worn in tick-prone environments. Eradication of high-risk areas includes maintaining lawns and surrounding shrubbery and extends to pet care and their protection.
Awareness includes education
Being aware of the propensity for Lyme disease infection in our changing climate encourages a preventative lifestyle that minimizes risk. Recognition of early symptoms allows for early medical attention and speedy treatment. Diagnostic accuracy within the medical community is also an important factor that will allow patients to undergo proper treatment with even the most unconventional presentation.
Support groups and online forums exist to allow patients with chronic symptoms to spread awareness and provide information on their recovery. Initiatives should continue to provide relevant and factual information about current symptoms, treatment, and preventative measures, as well as the eventual introduction and roll-out of vaccines into our communities.




